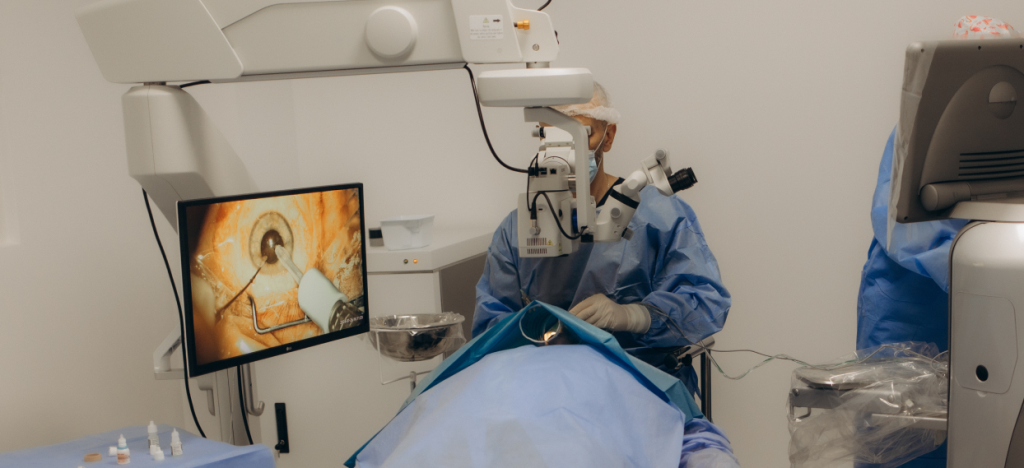
Everything You Need to Know About Intravitreal Injection Therapy
Intravitreal injection therapy, as it is known in medical terminology, involves the direct injection of medication into the vitreous cavity of the eye using a very fine needle. This allows the medication to reach the target area, the retina, in the shortest and most effective way possible.
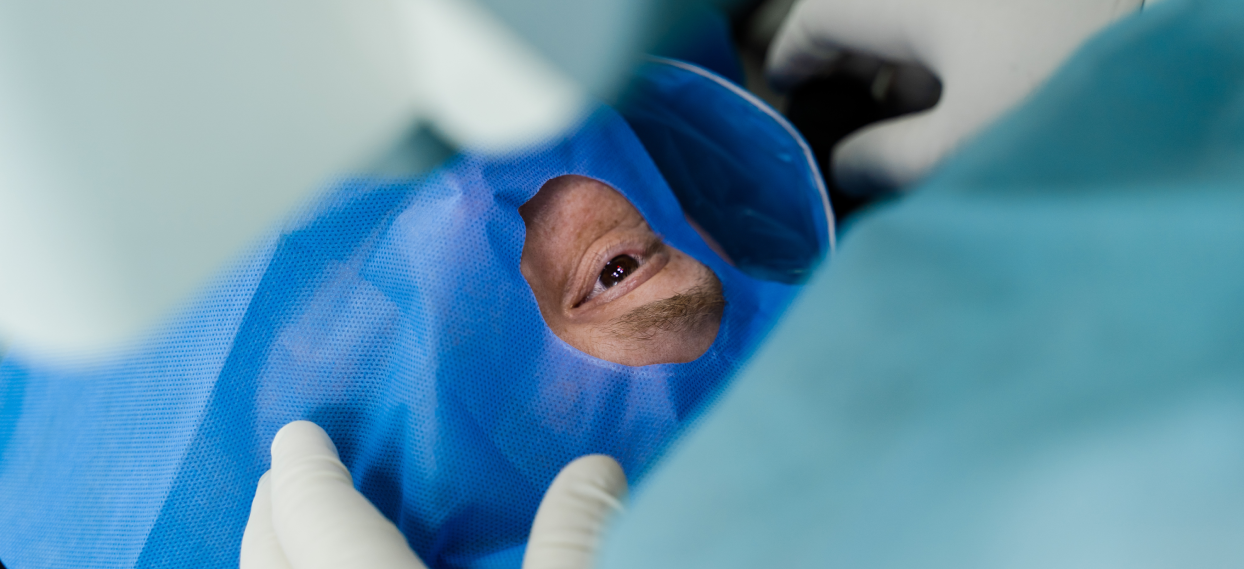
It is not difficult to imagine what goes through your mind when you first hear the words ‘We are going to inject a needle into your eye.’ Most people pause at this point and even consider postponing the treatment.
Yet intravitreal injection therapy, contrary to the frightening connotation in its name, is an extremely brief, controlled, and manageable procedure. Moreover, for many serious eye diseases, this treatment is the only way to save vision or preserve existing vision.
In this article, we will cover intravitreal injection therapy in all its aspects. We will explain how it is performed, in which situations it is applied, and answer some critical questions that most competing websites skip; because the real issue is not the needle itself, but the role and significance of this treatment in your life.
What Is Intravitreal Injection Therapy?
Intravitreal injection therapy is the medical term for what is commonly referred to as an eye injection. As the name suggests, the medication is directly injected into the vitreous cavity of the eye using a very fine needle. This allows the medication to reach the target area, the retina, in the shortest and most effective way possible.
Why is such a direct route necessary? Because the eye forms an extremely selective barrier against medications administered from the outside. Tablets taken orally or medications applied in the form of eye drops cannot reach the posterior layers of the eye in sufficient doses.
Eye drops only affect the anterior surface of the eye. The most reliable way to deliver medication to sensitive tissues at the very center of vision, such as the retina and macula, is through this injection into the vitreous cavity.
In Which Diseases Is It Applied?
Intravitreal injection therapy is used in the treatment of not just one, but many different retinal diseases. The main areas of application can be listed as follows:
- Retinopathy of prematurity: Retinal vessels that develop abnormally in premature infants can be brought under control with this treatment.
- Age-related macular degeneration (wet type): Abnormal and fragile vessels develop beneath the retina; fluid and blood leaking from these vessels damage the center of vision. The injected medication stops this leakage.
- Diabetic macular edema: Fluid leaks from retinal vessels due to diabetes mellitus, causing edema at the point of vision. Intravitreal injection therapy reduces this edema.
- Retinal vascular occlusions: Occlusion of the retinal vein causes edema and hemorrhage at the center of vision. Injections are also used effectively in this disease.
- Choroidal neovascularization due to high myopia: Abnormal vessel formation beneath the retina can occur in individuals with advanced myopia.
- Uveitis-related macular edema: In edemas developing as a result of intraocular inflammation, steroid-based injections are preferred in particular.
Which Medications Are Used in Intravitreal Injection Therapy?
Not all injections are performed with the same medication. The medication to be used is selected according to the diagnosis and the patient’s clinical condition. The main medication groups are as follows:
- Anti-VEGF agents: VEGF stands for vascular endothelial growth factor. These medications, which inhibit abnormal vessel formation and the leakage originating from these vessels, include molecules such as bevacizumab, ranibizumab, and aflibercept. They are frequently preferred in age-related macular degeneration, diabetic edema, and vascular occlusions.
- Steroid (corticosteroid) injections: These are used particularly in diabetic macular edema and uveitis-related edemas where a sufficient response to anti-VEGF therapy cannot be achieved. The dexamethasone implant is the most common example of this group and maintains its effect for 3 to 6 months.
- Antibiotic or antifungal agents: In cases of intraocular infection (endophthalmitis), it may be necessary to administer medication directly into the vitreous cavity.
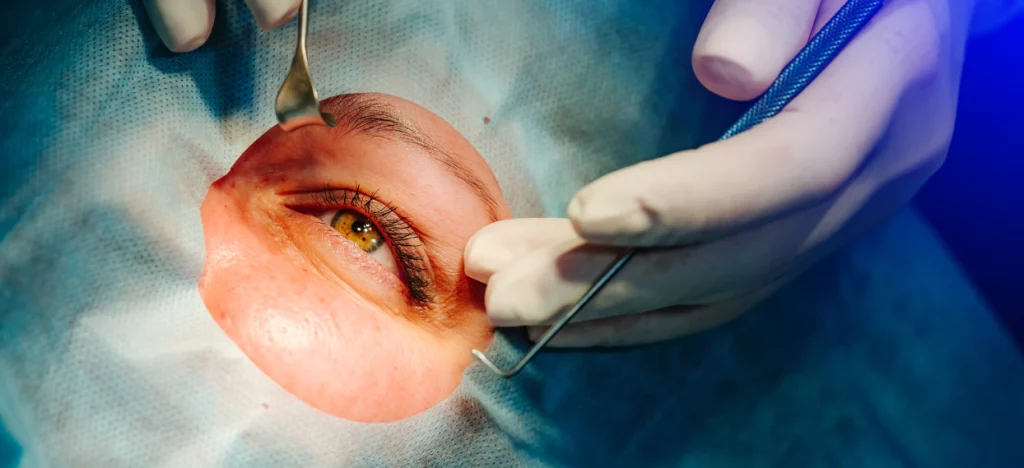
How Is Intravitreal Injection Therapy Performed?
Knowing how intravitreal injection therapy is carried out most often reduces anxiety. The process works as follows:
- Anesthetic drops are instilled into the eye, so no pain is felt throughout the procedure.
- The area around the eye and the eye surface are carefully cleaned with an antiseptic solution.
- A special instrument may be used to keep the eyeball steady.
- The needle enters through the white part of the eye (sclera), just outside the colored part of the eye (iris); this area lacks pain-sensitive nerve endings.
- The medication is delivered into the vitreous cavity within seconds.
- The procedure, including preparation, is completed in approximately 5 to 10 minutes in total.
Most patients describe only a mild sensation of pressure or fullness during the procedure. A genuine pain experience is extremely rare.
What Happens After the Procedure?
Let us address this stage in detail, which most competing websites gloss over but is very important for patients:
- On the day of the procedure: Mild redness and a stinging sensation in the eye are considered normal. This is related to the injection needle passing through the scleral tissue and generally resolves within a few days.
- Use of eye drops: The antibiotic drops prescribed after the procedure must be used regularly and without interruption. These drops play a critical role in preventing possible infection.
- Do not rub the eye: Rubbing the eye or applying any pressure in the first days following the procedure is absolutely inadvisable.
- When does vision improve? This is a very frequently asked question. The primary aim of intravitreal injection therapy is to halt the progression of vision loss rather than to improve vision. In some patients, vision improves noticeably within weeks, while in others recovery progresses more slowly. Each patient’s response must be evaluated individually.
- When should you go to the emergency room? If sudden and severe pain in the eye, a rapid increase in vision loss, intense redness in the eye, or excessive sensitivity to light develops after the injection, a physician must be consulted without delay. These may be signs of intraocular infection (endophthalmitis) and require extremely prompt intervention.
Is the Treatment a One-Time Procedure or Does It Need to Be Repeated?
This is one of the questions patients are most curious about and unfortunately one of the least answered. The honest answer is that it is usually not a one-time procedure.
In age-related macular degeneration, treatment is generally initiated with monthly injections in the first months; after 3 consecutive injections, the response to treatment is evaluated and a personalized plan is established. In patients who respond well to treatment, the intervals can be gradually extended; in fact, after a period of time, some patients may be placed on an injection-free follow-up process. However, if the disease relapses, returning to injections may be necessary.
A similar process applies in diabetic macular edema as well; regular injections may be required during periods when the disease is active. Discontinuing treatment early increases the risk of losing the vision that has been gained.
In short, intravitreal injection therapy is not a process that is carried out once and then concluded, but one that is sustained by closely monitoring the course of the disease. Missing follow-up examinations is a strong candidate for being the weakest link in this process.